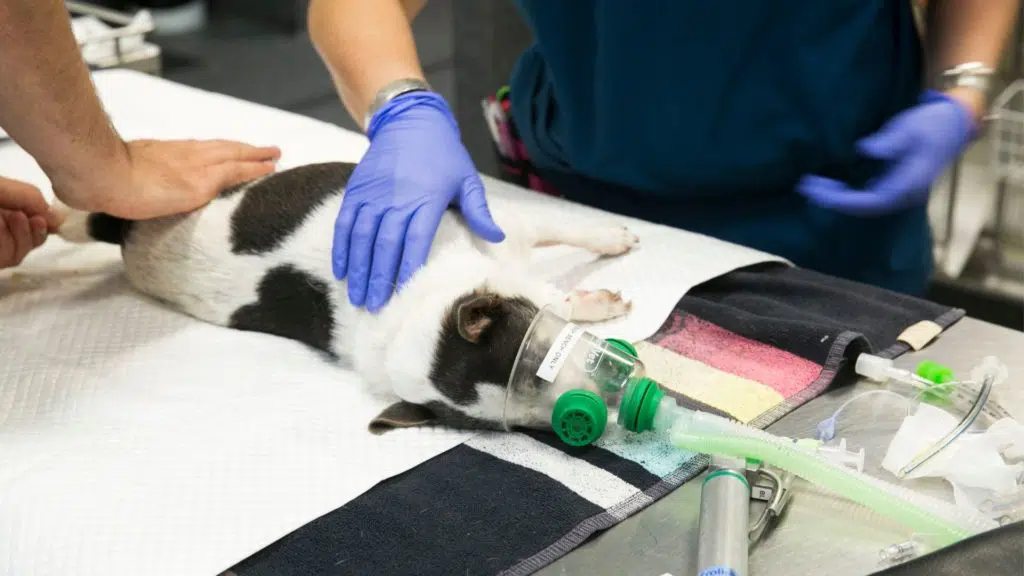
Feline Lower Urinary Tract Disease (FLUTD), formerly Feline Urologic Syndrome (or “blocked cats” as we commonly refer to them as), is typically seen in 1 – 7-year-old indoor and overweight male cats. More recently, this condition has been associated with a stressful event or environment leading to changes in the patient’s urogenital tract, not to mention inflammatory signalling and gastrointestinal status.
Though there is no single leading cause, contributing factors have been attributed to a longer and tapering urethra compared to females, formation of distal plug from inflammatory components (mucus, protein, cells), uroliths, crystalluria, infectious vs sterile cystitis, and increased sympathetic tone to the proximal urethra. Despite these, the majority are identified as idiopathic and given the name Feline Idiopathic Cystitis (FIC).
Feline Lower Urinary Tract Disease – Pathophysiology
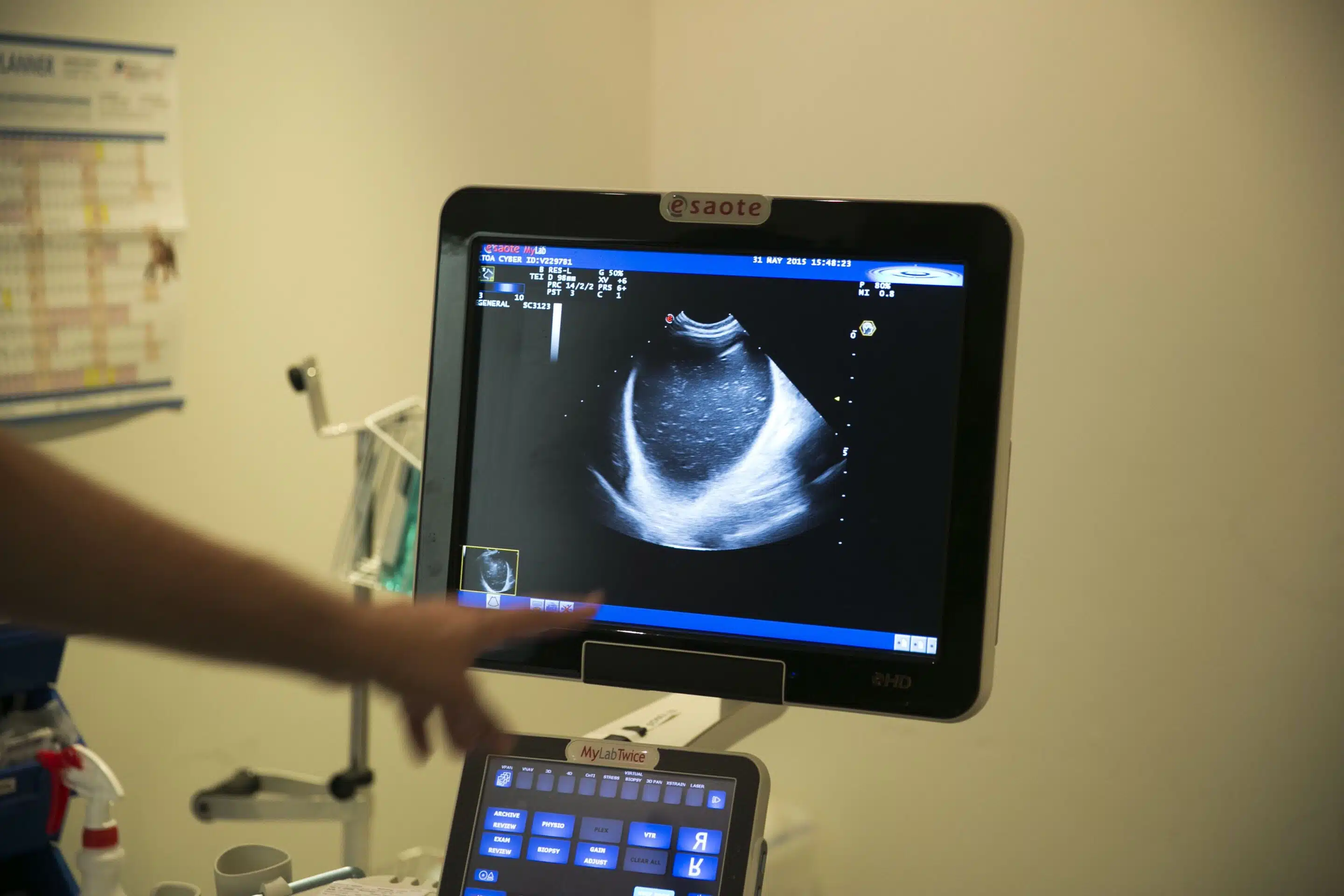
On presentation, FLUTD is typically associated with immediate palpation of a distended bladder, however, this can vary in size between males and sometimes a FAST abdominal ultrasound is required. More importantly, though, establishing the patient’s cardiovascular status should take priority due to the bradycardia effects from hyperkalemia (HR<160) and acidemia from possible uraemia (ie: post-renal azotemia) due to a reduced glomerular filtration rate (GFR).
If severe enough (K>9mmol/L), asystole can occur and rapid myocardiocyte stabilization is required. The effects of bradycardia are considered 2-fold, a reduction in cardiac output and reduced organ perfusion, and its compensatory increase in sympathetic drive and vascular tone, resulting in improved pressure but reduced blood volume, both of which reduce GFR further.
Clinical Signs
- Tachycardia (HR>220) or,
- Bradycardia (HR<160)
- Vomiting
- Stranguria
- Haematuria
- Pollakiuria
Diagnostics
- PCV/TS
- Electrolytes (Na and K particularly)
- Biochemistry
- Urinalysis (once unblocked)
- Ultrasonography
- +/- Radiography
The reduction in GFR consequently leads to a direct reduction in renal tubular flow and other electrolyte abnormalities. Once relieved, normal kidney function typically resumes, though post-obstructive diuresis (POD) can occur (polyuria). This latter process is not well understood, though is possibly related to osmotic diuresis from elevated urea, high tubular sodium and water retention, and the inability for ADH to have an effect from loss of the medullary concentration gradient as a result of increased tubular flow after relief of the obstruction. Urine output (UOP), ins/outs and frequent weighing of the patient are required to ensure the patient maintains normovolaemia.
Regardless of the cause and ease of unblocking the urethra, the recommendation is to leave the urinary catheter in place for at least 24hrs. This allows time for the reduction of inflammatory effects on the bladder wall, reduction in effects of sympathetic drive, monitoring effects of possible POD, reduce crystalluria, and allow a change in urinary characteristics from possible infection. It is well-known struvite crystals form in alkaline and high Magnesium (Mg) environments, and a high suspicion for infectious cystitis should be considered as urease-producing bacteria cleave urea to ammonia causing an increase in pH.
Treatment of the Stable Feline Lower Urinary Tract Disease Patient
Classification of a stable FLUTD patient: K <6.5mmol/L, no vomiting, HR >160
- Provide analgesia on presentation
- Methadone 0.2-0.3mg/kg IM
- Buprenorphine 0.02-0.03mg/kg IM or IV
- Fluid therapy
- Bolus crystalloid fluid as required (approx. 5-10ml/kg initially and reassess)
- Provide at least 1-2hrs fluid therapy prior to giving an anaesthetic agent
- Anaesthesia +/- Sedation
- Fentanyl 3-5ug/kg IV (0.3-0.5ml/5kg Cat, assuming 50ug/mL) + Midazolam 0.2mg/kg IV (0.2ml/5kg Cat, assuming 5mg/mL) – same syringe (PREFERRED)
- Ketamine 2-4mg/kg IV (0.1-0.2ml/5kg Cat, assuming 100mg/kg) + Diazepam 0.3mg/kg IV (0.3ml/5kg Cat, assuming 5mg/ml) – same syringe (NB: only if NO Cardiac concerns)
- Induce with alfaxalone (5-15mg IV) and intubate. Maintained with 1-2% isoflurane, FiO2 100% at 1L/min

Treatment of the Unstable Feline Lower Urinary Tract Disease Patient
Classification of the unstable FLUTD patient: K >6.5mmol/L, vomiting, obtunded, HR <160
- Place IV catheter immediately
- Analgesia – care with contributing to worsening demeanour/respiratory drive
- Methadone 0.2-0.3mg/kg IM, or
- Buprenorphine 0.01-0.02mg/kg IM or IV
- Treat Shock – LRS or 0.9% NaCl up to 40-60ml/kg/hr for ¼ shock rate volumes (i.e., 10-15ml/kg boluses)
- Treat Hyperkalaemia – monitor with ECG during treatment
- Calcium Gluconate 10%: 1ml/kg over 10 minutes (max effect in 3-5mins)
- Glucose: given at 0.5g/kg (1ml/kg 50% glucose diluted 1 in 4) (max effect in 30mins)
- +/- Insulin: 0.25-0.5 IU/kg IV or IM (C2) (max effect in 30mins)
- NB: glucose MUST have been given first
- NB: 2.5% Glucose MUST be added to IV fluid (50ml of 50% added to 1L crystalloid)
- +/- NaHCO3 (Sodium Bicarbonate): 1ml/kg (only if absolutely necessary), pH <7.2 and HCO3 <12 (max effect in 15mins)
- Provide appropriate sedation to relieve urethral obstruction and place indwelling urinary catheter under
- Avoid isoflurane due to vasodilating effects on an already CV compromised patient
- Fentanyl 3-5ug/kg IV (0.3-0.5ml/5kg Cat, assuming 50ug/mL) + Midazolam 0.2mg/kg IV (0.2ml/5kg Cat, assuming 5mg/mL) – same syringe (PREFERRED)
- Ketamine 2-4mg/kg IV (0.1-0.2ml/5kg Cat, assuming 100mg/kg) + Diazepam 0.3mg/kg IV (0.3ml/5kg Cat, assuming 5mg/ml) – same syringe (only if NO Cardiac concerns)
- +/- Alfaxan PRN (1-2mg IV boluses as required)
- Provide flow-by oxygen during the procedure due to mild hypoventilation and have intubation equipment ready
- Do not administer anaesthetic if moribund on presentation
Urinary Catheter Placement
Placement of a urinary catheter and relieving the urethral obstruction is arguably the most vital component of treating feline lower urinary tract disease. Below we outline a step-by-step guide to urinary catheter placement to ensure you can successfully unblock your patient and reduce the risk of recurrence.
- Place the patient in dorsal vs lateral decumbency and clip perineal and preputial area and clean with aqueous chlorhexidine (0.05%), flush penile tip/prepuce with 3x with 5ml of aqueous chlorhex
- Pull the back legs cranially or keep as lazy caudal
- With sterile gloves on, expose the penis tip and instil 2% Lignocaine gel into the prepuce
- Use a 20-22g IV Catheter tip and 10ml sterile saline solution to flush the tip of the penis
- Avoid excessive catheterization due to the risk of urethral trauma/tear and stricture formation
- Never perform cystocentesis on a distended and stressed bladder wall for risk of rupture
- If the obstruction is not in the tip, then flush the entire urethra with a TomCat catheter (do not use it as an indwelling catheter).
- Make sure you straighten the urethra (once 2-4mm inside urethra pull prepuce caudally, then dorsally in parallel with the tabletop to straighten out the urethra)
- Place 2% Lignocaine gel throughout the length of the urethra with the TomCat catheter
- Place a 3.5FR x 12-14cm indwelling TomCat indwelling Urethral catheter/attach Little Herbert and secure in place to prepuce
- Do not use a stiff Tomcat or feeding tube as an indwelling due to risk of pressure necrosis.
- Slippery Sam TomCat catheters are known to separate under duress and can be lost into the bladder
- Flush the bladder with 20ml warm saline until it runs clear (remember to ‘jiggle’ the bladder as performing flushing)
- Attach secured closed collection system and secure to the tail. Allow for tail movement and possible pulling at the prepuce
- Leave urinary catheter in place for at least 24hrs if marked initial bladder distension to prevent further bladder wall trauma
NB: urinary catheters will cause irritation to the urethra and urothelium and subsequent haematuria, so removal as early as possible is preferred, though without compromising morbidity from recatheterisation if removed too early.
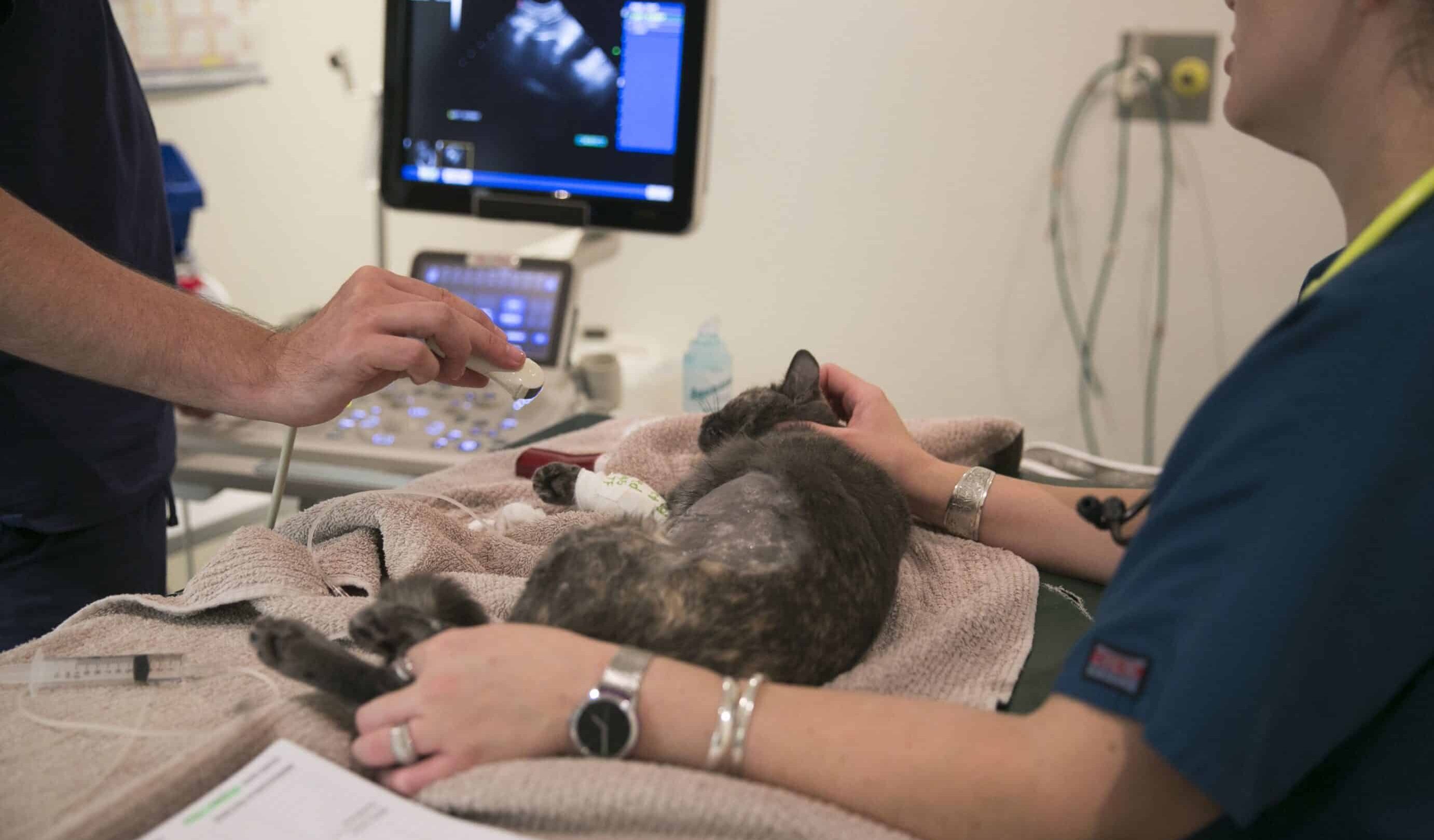
FLUTD Treatment – Medications
- Analgesia
- Buprenorphine 0.01-0.02mg/kg IV or SL q8-12hrs
- Muscle relaxants: started 24-36hrs after urinary catheter is placed only (reduced rate of recurrence within 24hrs, 18% compared to 24%)
- Dantrolene 1mg/kg PO q12hrs for 7 days (skeletal muscle)
- Prazosin 0.5mg PO q12hrs (0.25mg if <4kg) for 7 days (smooth muscle)
- Do NOT use phenoxybenzamine (increased recurrence rate vs no meds)
- Anti-inflammatory (NSAID or steroid) – consider using if CVS stable 30min prior to removal of urinary catheter to reduce inflammatory effects on bladder wall only (no change to recurrence rate or duration of hospitalization)
Additional Treatment and Monitoring
- Fluid therapy: initially 5-10 ml/kg/hr if euvolaemic & no contraindications then modify on the basis of urine output, PCV/TS, electrolytes and hydration status.
- Modify IV fluid rate to exceed urine output (for a 5kg cat, 5% dehydration = 10 ml/kg/hr). May require higher IV fluid rates as long as patient’s cardiovascular and respiratory status tolerates it. Reassess this rate regularly.
- TPR q4hrs initially, then extend to q6hrs
- Assess urine output q4hrs
- Monitor weight q4hrs due to risk of post-obstructive diuresis
- Post-obstructive diuresis is an abnormally high UOP (outs>ins) that continues for 12-24 hours after bilateral ureteral blockage. Unknown cause, but patients can become hypovolaemic if not monitored closely
- PCV/TS/electrolytes q8-12hrs
- Perform sooner if concerned about obstructive diuresis vs acute kidney injury vs hyperkalemia on presentation.
- Feed wet food only and allow access to fresh water at all times (NO biscuits)
- c/d or s/d preferred. Consider kangaroo, tuna, sardines, fish (60-70% water content).
- Place the patient in a quiet, dark environment and spray cage with Feliway
- Leave urinary catheter in for at least 24hrs until urine is clear
- Diagnostic imaging should be recommended to the owner at admission (i.e., R Lat radiograph and US for uroliths vs neoplasia)
- 90% sensitivity if combined (77% US if used alone)
- Consider the need for analgesia and anti-inflammatory drugs
- Whilst the patient is in hospital, perform urinalysis at catheter placement (t=0) and then every 24hrs to monitor for possible bacteriuria and pyuria.
- Start antibiotics (i.e., cephalosporin) as indicated if bacteriuria is present and send away urine for MC&S
- Bladder size must be checked prior to discharge and transfer to the primary vet for ongoing management
- Avoid antibiotics (unless bacteriuria confirmed), prolonged corticosteroids or bethanechol
- Consider sending urine for MC&S on presentation and including after catheter removal
- Bacteriuria reported in 33% cats with urinary catheter in place >48hrs
FLUTD Prognosis and Risk Factors
The recurrence rate for feline lower urinary tract disease is 24% 24hrs following discharge (22% reported at 6mths). This is reduced to 18% if Prazosin is given prior to discharge. This is also reduced if 3.5FR is used over 5FR catheter size and the urinary catheter is left in place >32hrs. However, bacteriuria also occurs in 33% of patients if the urinary catheter is kept in place longer than 48hrs.
Feline Idiopathic (Interstitial) Cystitis is the most common reason for an obstruction (50%), followed by urethral plugs (25%), uroliths (20%) (Struvite vs Calcium oxalate), infection, urethral spasm, neoplasia (e.g., TCC, LSA), abdominal mass, pelvic/sacrocaudal fractures, neurogenic (dysautonomia), diverticulum, or iatrogenic. If the patient is >10yrs old, the risk of neoplasia as a causative agent increases dramatically.
There is a significantly increased risk of FLUTD developing if the patient’s weight is >5kg, has access to fewer litter trays and allowed to remain indoors. In these cases, it may be necessary to consider referral for Perineal Urethrostomy if feline lower urinary tract disease occurs a third time.
To find out more about Feline Lower Urinary Tract Disease and download a handy print-out protocol to keep in your clinic, visit VetAPedia for 100+ free clinical resources. And for more emergency content, be sure to check out our emergency guides, including our guide to anaphylaxis and our series of tick paralysis articles.