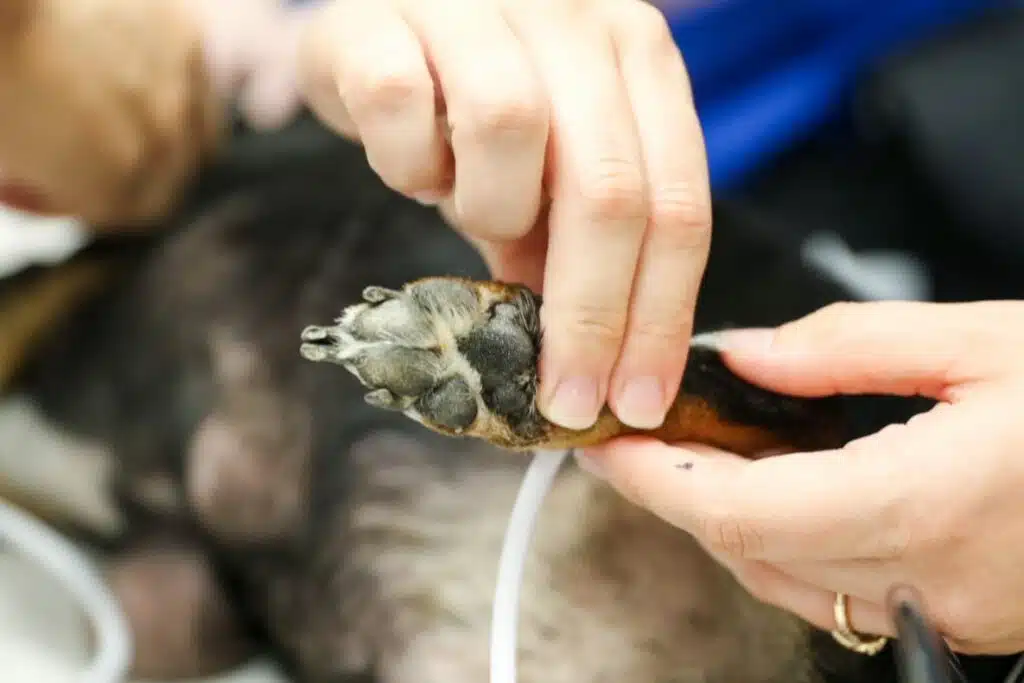
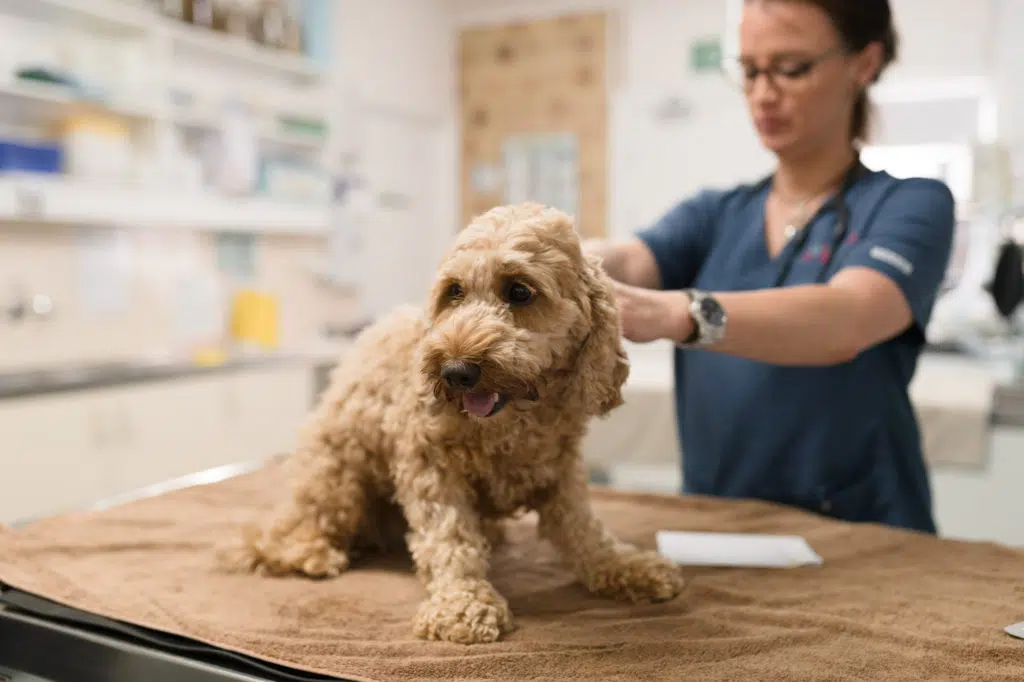
When creating our webinar on Transitioning from Uni to Emergency as a New Grad, in order to truly prepare you to transitioning into emergency practice, we wanted to ensure you were first able to understand two vital components: what emergency practice is like, and what is it like to be think like an emergency veterinarian. To help you understand this, join Dr Gerardo from Animal Emergency Australia and watch our webinar below to explore the 7 key differences between GP and emergency veterinary practice.
Generally, emergency veterinarians feel like they are like circus performers who have to “spin stacks of plates, one on top of another, of all different shapes and weights”. This can be further complicated by simultaneous demands from multiple parties: from patients, the clients, and even surrounding team members and colleagues.
Added to that is the time-bound interventions and parallel tasks required. So putting it all together, emergency practice can be thought of no less than being chaotic. The main explanation for this is that emergency veterinarians are seen to act immediately on their patients when other fields of veterinary medicine may take longer or have more time to prepare and decide on what action to take.
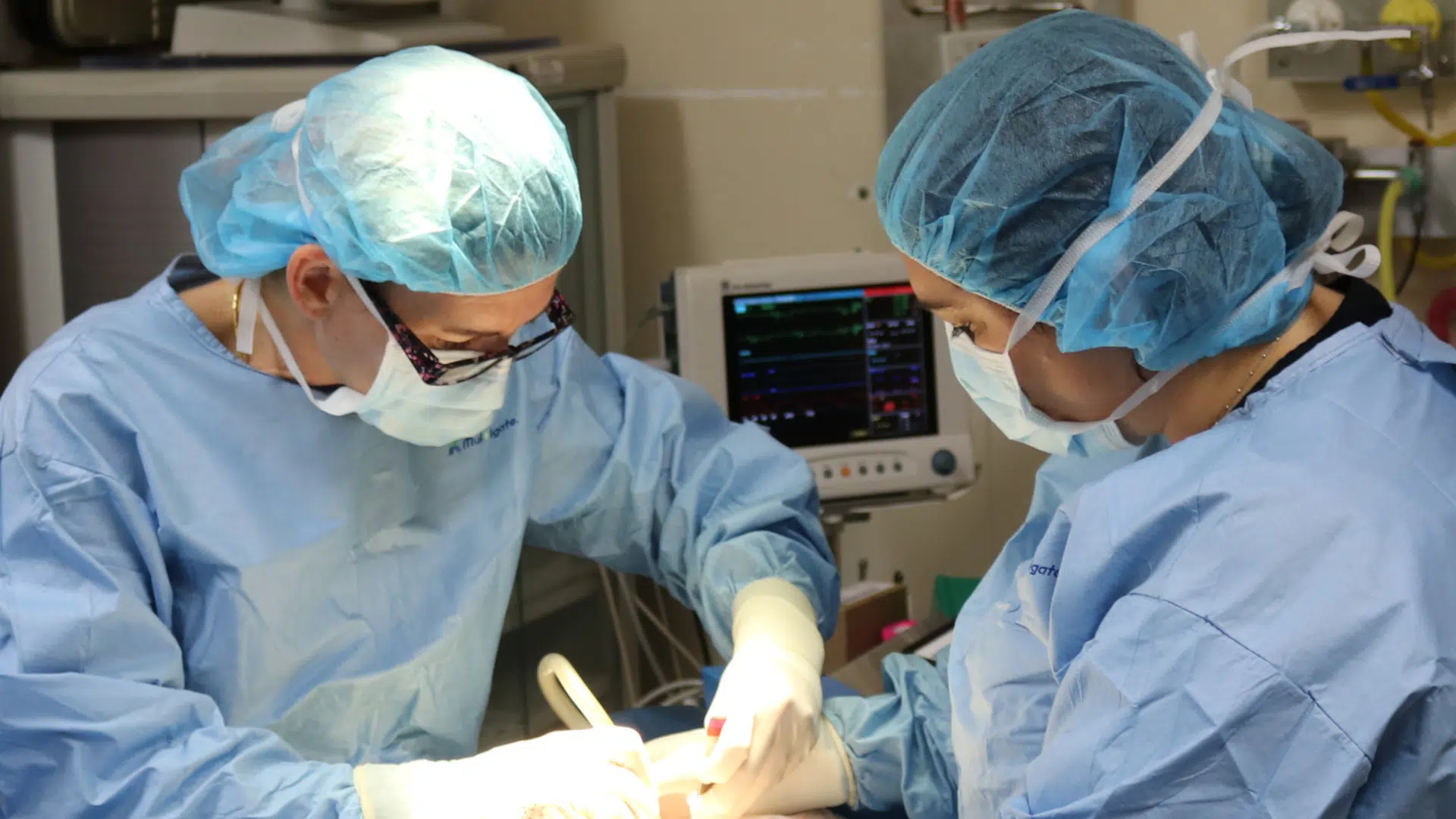
To break this down further, this article explores a general comparison of the differences between GP and emergency veterinary practice. When referring to general practice, it’s not just small animal. These characteristics also apply to large animal and specialty practices, which we’ll instead use the term “general medicine”. Both emergency and general medicine are on two completely different spectrums in many ways.
So read ahead to discover the 14 characteristics that differentiate the two, which have been merged into 7 main groups of related characteristics. This will help you create a better picture of the differences so that you get a better understanding of whether emergency is for you, and if so, how to prepare for it.
The 7 Key Differences Between GP and Emergency
1. Structure, Dynamics, and Flow of Process
General medicine: More structured and planned, generally you have set appointments where you and plan and structure the day. This means there is less requirement on you to be dynamic. Case work can be mostly be planned and prepared for, it is mostly linear, one thing at a time.
Emergency medicine: There is little structure, you have no control over what comes in and you don’t know what is coming in and when. This results in a higher requirement on you to be dynamic and adjust and shift with what is happening around you. Case work can be multi-directional rather than linear, where you are often assessing multiple different things and multiple cases at once.

It’s important to also realise that multitasking is a myth. It’s not multitasking, it’s task switching. Emergency medicine requires you to be able to switch between one task and the next, from one patient to the next, then back to the original patient. Some people find this haphazardness confusing and overwhelming, but you can create a system where you keep track of your patients, where they are at and what is happening next.
Task switching can be as simple has having your patients on a clip board, that you constantly review, check in with the nurses, review the response to stabilisation, review the diagnostics that come through. Then plan the next step, so that even though you are jumping back and forward and left and right, you can still keep track. Utilising task switching to the best of your ability is one of the vital differences between GP and emergency practice.
2. Client Interactions and Relationships
General medicine: Generally, the client has a previous history with the practice. Clients are less stressed or worried, and are more prepared. They also have more time to decide, meaning there is more time to cultivate or develop a lasting relationship which is ongoing.
Emergency medicine: Generally, no prior relationship exits and unlike general medicine, there is limited time to cultivate a lasting client relationship. Instead, the goal is to stabilise and manage the primary presenting problem. Clients are more stressed, worried and unprepared. There’s also less time to decide, meaning client relationships rarely continue after the visit.

If you follow the right mentors or have the right supervisors, you’ll soon see the style of communication that is effective in terms of obtaining the key information that you need in less than a minute. You’ll also be able to intervene whilst still being empathetic, building connection and trust. Within emergency medicine, clients often know that you need to intervene immediately and they also communicate in a direct and concise manner. So once the patient is stable, a longer and more detailed discussion can be had.
3. Information Gap
General medicine: Less of an information gap, as there is either previous history or able to obtain a complete history. Vets within general medicine will also have the opportunity to perform a full physical exam or more time to gather information before intervention is required.
Emergency medicine: More of an information gap is present, as there is either no previous history or less time to gather the history. There may not be adequate time to perform a full physical examination, or to gather more diagnostic information before intervention is required.

Generally, emergent patients have a very short or acute history, they present with “worst case scenario” types of diseases (e.g., trauma, GDV, wounds, severe acute vomiting). So your interventions are generally focused on ruling out worse case scenario diseases due to limited information. Depending on the emergency practice, a lot of diagnostics may be done to investigate for those diseases. So diagnostic tests are instead screening for worse case scenario diseases, rather then being more focused on diagnosing a particular disease.
4. Time Available & Degree of Intervention
General medicine: It can be very busy, but you often have more time to decide what to do and when, as the patients are more stable. There’s less requirement on you to be immediately interventional, with more of a preventative or prophylaxis style of medicine.
Emergency medicine: It can also be very busy, and often you have very little time to decide what to do because patients are less stable or critical. There’s instead a higher requirement for you to intervene immediately, with very little preventative style of medicine.

Being able to decide what to do with limited time is very difficult as a new graduate, that is why a structured program with the right support will set you up for success. You can only really learn what interventions are required and appropriate through watching others, applying it yourself, and through applying frameworks and processes that only really make sense when you are standing at the triage bench. You can have all the knowledge in the world, but application in real practice with guidance is the real way of cementing it.
5. Action vs. Analysis
General medicine: Generally primed for analysis, gathering more information. The focus is on determining a diagnosis, as patients are more stable.
Emergency medicine: Generally primed for action, information initially is geared at ruling out worst case scenarios for common presentations because there is less information available and patients are more critical.
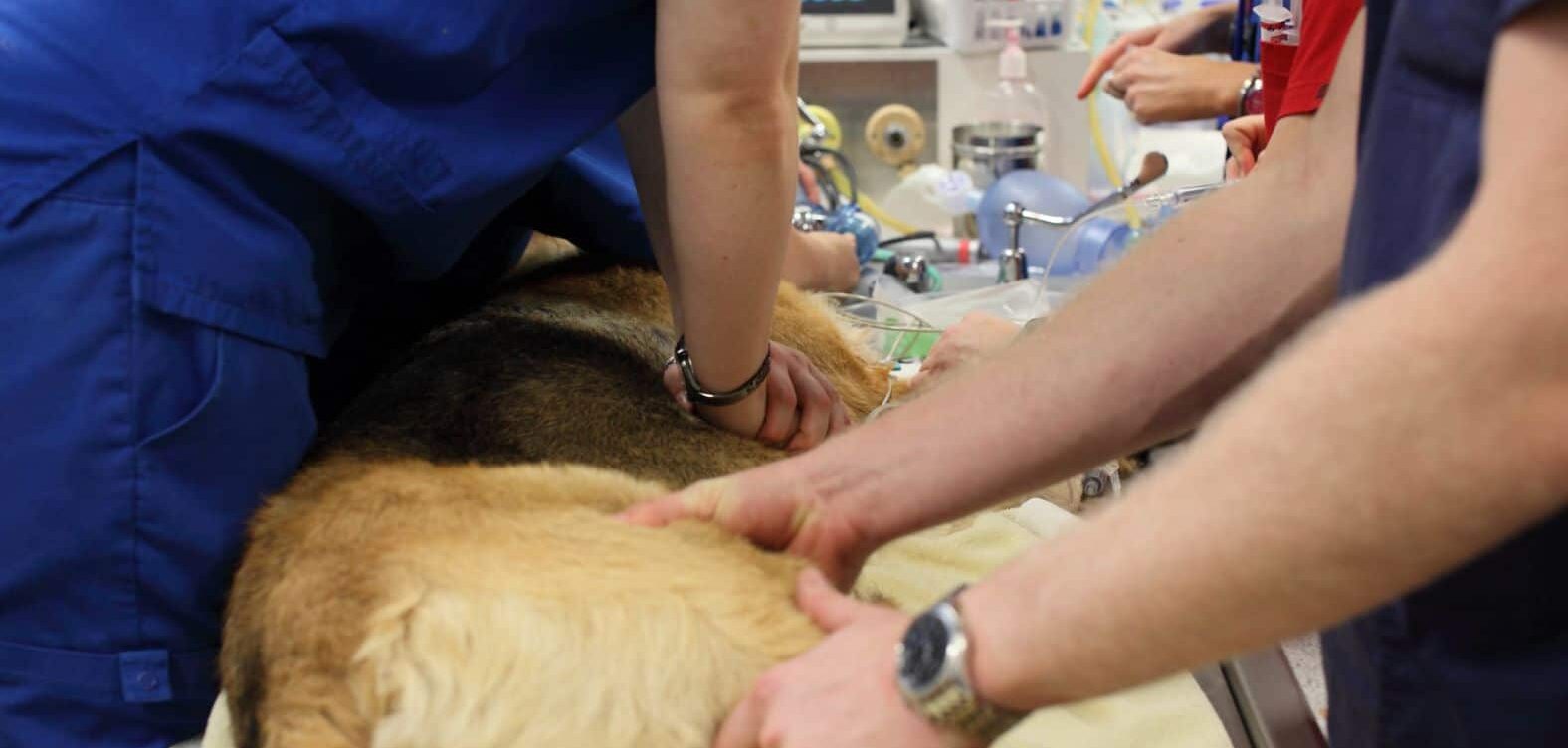
Being primed for action is hard, and being ready to intervene again comes down to application of frameworks and processes (e.g., CPR process, triage process). Simply being prepared is important too, or just knowing that sooner or later you will make the wrong call, it will just happen. However, you learn from the process, and generally the interventions are rarely catastrophic or result in death, which provides leeway.
6. Targets and Stakes
General medicine: Targets are generally about determining a diagnosis and working out the best option. As a result, the stakes are lower.
Emergency medicine: Target is to assess, triage, manage acute life-threatening conditions. Emergency clinicians must perform the best workable options based on worst case scenarios, and when stable, determine the next best workable options and potentially a diagnosis. So naturally, in these situations, the stakes are higher.

You have to be comfortable with being uncomfortable, or being not 100% certain and also with high stakes. It even took Dr Gerardo a couple years to be ok with that, so you have accept that it comes with the job. Over time with the right support, guidance and experience, it will become less and less uncomfortable.
7. Case Load and Complexity
General medicine: Generally, general medicine settings will see a larger number of patients. This could range between 15 to 30 patients a day, most of which will be less complex and less critical cases.
Emergency medicine: This depends on the emergency practice and the style of medicine. Some emergency hospitals see more patients that are less critical or don’t work patients up to a diagnosis, as they may leave that to the medicine team or the referring vet the next day. However, some hospitals see a lot more critical patients and their style is geared towards determining a diagnosis rather than managing symptomatically. In these hospitals, the vets would see less patients per vet.

Here at AEA, our hospitals we are busy, meaning we have more vets on as we are referred more complex cases. This varying case load can be one of the most significant differences between GP and emergency practice. Our style of emergency works towards a diagnosis and our hospitals perform their own own emergency surgeries. As a result, we see less patients per vet (for example 6 – 10 cases, rarely up to 15).
Overall, there are many differences between GP and emergency! Even just the clinical decision-making in emergency care requires a unique approach that is distinctive to the emergency environment. It often takes a full shift in mindset to transition from general practice to emergency.
The unplanned nature of emergency brings with it uncertainty, requiring professionals to work on multiple and concurrent tasks, whilst accepting the uncertainty. The complex emergency environment requires all emergency clinicians to accommodate the factors we’ve discussed to form a timely and priority-based, situationally adaptable approach.
Now that you know the differences between GP and emergency, do you want to find out more about transitioning to emergency? Join our team of veterinarians from AEA who have made the step from uni to emergency as they discuss the traits of successful emergency vets in our next article: Should You Choose Veterinary Emergency?
Download Your Free GP vs. Emergency Infographic
GP vs. Emergency Mindset
Download your vet mindset infographic.