Anaphylaxis in dogs and cats is an immediate, severe and potentially life-threatening hypersensitivity reaction to an allergen (antigen). Before a reaction like this can occur the animal must have had previous exposure to this allergen. Any foreign substance can potentially cause an allergic reaction but the most common substances are insect bites. Other causes include food proteins, medications, vaccines, environmental pollutants and chemicals.
Knowing how to recognise and respond to anaphylaxis in dogs and cats can be incredibly helpful for all veterinary professionals. This can be one of the most common emergency presentations seen in clinical practice! In this article, we’ll give an overview of the pathophysiology behind anaphylaxis, take a closer look at its clinical signs and how you can diagnose it, and then provide you with the most effective options for treatment. So grab that adrenaline vial and let’s find out all about anaphylaxis in dogs and cats!

Pathophysiology of Anaphylaxis in Dogs and Cats
In immune-mediated anaphylaxis, previous exposure to an antigen results in sensitization and IgE is produced. This is bound to the cell surface of mast cells and basophils. With repeated exposure, the antigen causes cross-linkage of two IgE molecules and the cell is activated. This releases biochemical and vasoactive substances such as histamine, pro-inflammatory cytokines, leukotrienes and tryptase.
Histamine and leukotrienes are potent vasoactive mediators and their release from eosinophils and basophils increases vascular permeability and vasodilation. Hypovolemia then results from plasma leakage into the interstitial space. Histamine acts on receptors to promote shock by causing coronary and systemic vasodilation, increasing heart rate and ventricular contractility.
Histamine also acts on receptors in the respiratory tract to cause rhinitis, pruritus and bronchoconstriction. Additionally, histamine stimulates endothelial cells to produce nitric oxide causing further vasodilation. The resulting hypotension and hypoxemia worsen cardiovascular collapse. Pro-inflammatory cytokines are then responsible for promoting the late-phase inflammatory response.
Typically, in dogs, the anaphylactic shock organ is the liver and in the cat, it is the respiratory tract. Dermal and ocular manifestations can occur in both species. In dogs, hepatic venous congestion is manifested in portal hypertension and visceral pooling of blood leading to vomiting and diarrhea. This venous congestion leads to gallbladder oedema and the formation of the ‘halo sign’ on ultrasound that is often (but not always) found associated with anaphylaxis.
Anaphylaxis in Dogs and Cats – Signs and Diagnosis
Given the widely variable clinical manifestations, anaphylaxis can be difficult to diagnose. The diagnosis is primarily based on a detailed history and the clinical presentation of the animal. As a result, being able to correctly diagnose anaphylaxis in dogs and cats can be highly dependent on pattern recognition.
In some circumstances, a visible puncture wound or an embedded stinger may be noted. Or occasionally an area surrounding a bite wound may show erythema or swelling locally. There may also be wheals present and the patient may be pruritic. These are typically pathognomonic for anaphylaxis, but will not appear in all cases.
Signs of Anaphylaxis in Dogs
- Vomiting/Diarrhea/Hemorrhagic diarrhea
- Collapse/Weakness
- Seizures
- Lacrimation/Conjunctival injection
- Hypovolemic shock
- Bradycardia (due to increased vagal reactivity)
Signs of Anaphylaxis in Cats
- Respiratory distress
- Hypersalivation
- Incoordination
- Vomiting
- Diarrhea/Hemorrhagic diarrhea
- Hypovolemic shock
- Hemoabdomen
Dermal Signs of Anaphylaxis:
These signs of anaphylaxis can occur in both species and include:
- Facial angioedema
- Severe Pruritus
- Localized erythema or swelling
- Wheals
- Urticaria
Laboratory changes may or may not be present. These can include thrombocytopenia, hemoconcentration, anemia, leukocytosis, elevated hepatic enzymes (most commonly ALT), hyperbilirubinemia, azotemia, hyperlactataemia, and mild prolonged clotting times.
AFAST ultrasound is commonly used to determine anaphylaxis in dogs and cats, as a Gall bBadder “halo sign” is the most common sign associated. Patients may also present with hemoabdomen which can be diagnosed on ultrasound.
Differentials for anaphylaxis in dogs and cats can include severe asthma, pheochromocytoma, vasodepressor events (vasovagal episodes), systemic mastocytosis, snake envenomation (Australia), syncope, thromboembolic event, and non-traumatic haemoabdomen.
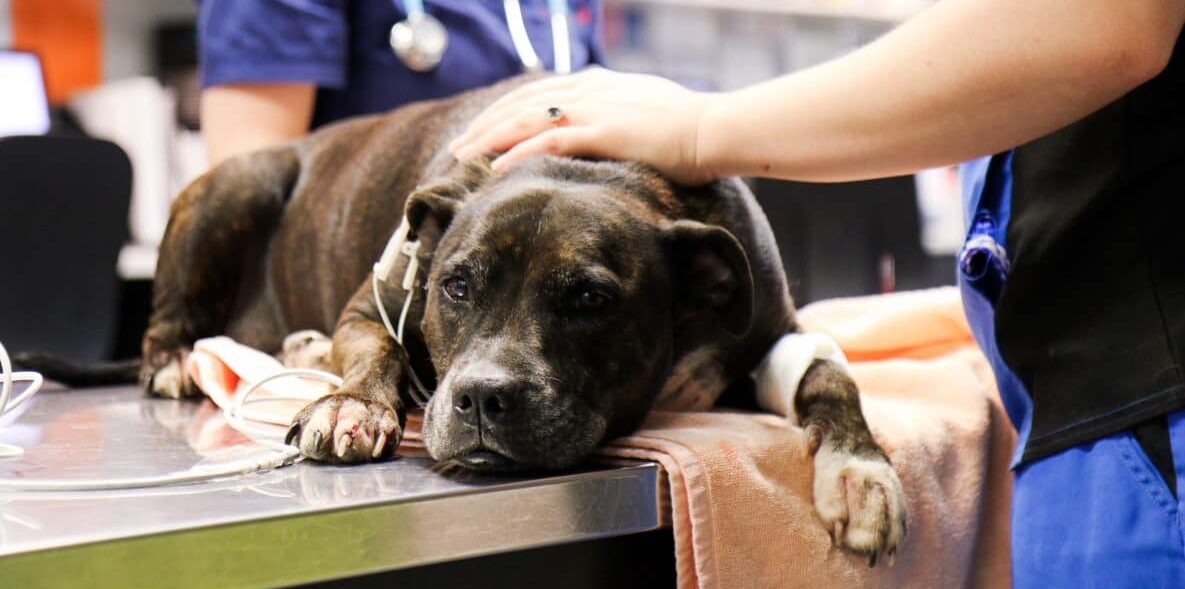
Treatment of Anaphylaxis in Dogs and Cats
Anaphylaxis is a life-threatening emergency and prompt recognition is vital to start life-saving treatments as soon as possible. Aggressive treatment should be initiated before diagnostics are performed since rapid deterioration is common. Treatment involves several useful medications to directly address shock and immune response. There are also a number of useful supportive treatments to help stabilise the patient.
Medications
- Epinephrine: 0.01mg/kg of a 1:1000 (1mg/ml) solution IM initially
- Depending on the severity of the signs this can be repeated every 15 minutes as necessary
- If the patient is already showing signs of shock, absorption from IM administration is unpredictable and unreliable, therefore an IV infusion should be instigated at 0.05 mcg/kg/min titrated to clinical response
- Antihistamines: treatment with H1 and H2 antihistamines combined has been reported to be more effective than treatment with H1 alone.
- Diphenhydramine (H1): 1-4mg/kg IM or PO TID in dogs, 0.5-2mg/kg IM or PO TID in cats
- Chlorpheniramine (H1): 0.5mg/kg IM q12hrs
- Ranitidine (H2): 0.5-2.5mg/kg IV PO or SC
- Dexamethasone: 0.1-0.4mg/kg IV
- Steroids are controversial in the initial emergency treatment of anaphylaxis since the risk of GIT ulceration and AKI is high if given when patients are not hemodynamically stable. Use with caution.
- Bronchidilators:
- Albuterol (salbutamol): 0.5mL of 0.5% solution in 4mL of isotonic saline by nebulizer every 6hrs or 90mcg/actuation (1-2puffs) by inhaler every 15 minutes up to 3 doses
- Aminophylline: 5-10mg/kg IM or slowly IV
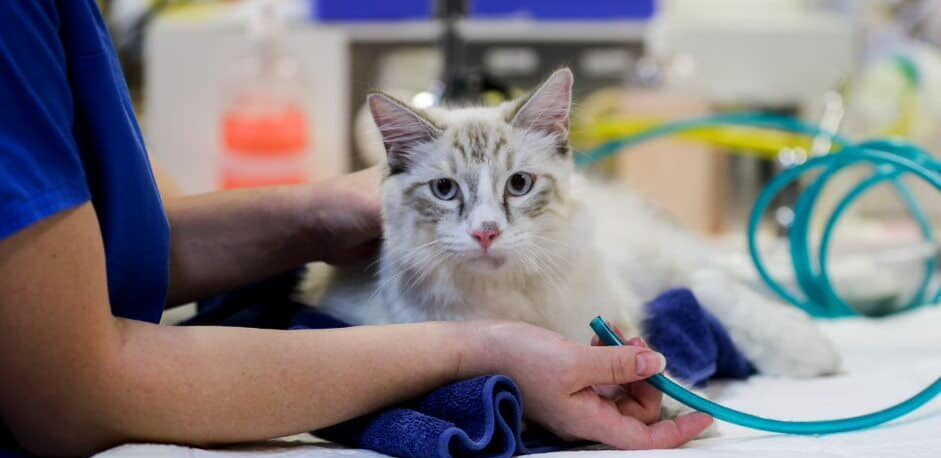
Supportive Care
Fluid resuscitation is vital, as within a few minutes of a severe reaction a significant portion of the blood volume extravasates. When combined with vascular pooling, this reduction in circulating blood volume leads to severe distributive shock. Resuscitative volumes of crystalloids should be given to prevent cardiovascular collapse. Boluses should be given while monitoring end point variables (mentation, heart rate, mucus membrane colour, capillary refill time, pulse pressure, temperature and lactate) and aiming for a systolic blood pressure of 100-120mmHg.
Oxygen support is also another mainstay of initial treatment, especially given the presence of shock causing decreased oxygen carrying capacity. High flow oxygen should be delivered to the patient until they are hemodynamically stable and until any signs of respiratory distress resolve.
Blood transfusion may also be necessary in some cases where patients develop coagulation issues, haemoabdomen or possibly DIC and occasionally plasma transfusion made be indicated to treat ongoing bleeding.
Management and Monitoring
Patients should be admitted to hospital for monitoring over the next 12 to 24 hours, as approximately 20% of anaphylactic patients can potentially have a biphasic reaction. This commonly occurs 8 to 12 hours after the initial anaphylaxis, but can be up to 72 hours. The clinical signs of the second reaction can be less severe, equally as severe or more severe than the initial reaction.
The optimal way of providing first aid treatment in people with anaphylaxis is the use of IM epinephrine via auto-injection (EpiPen). This has not been well investigated in veterinary patients and given the current fixed dose pens available, is not overly useful for any patients weighing less than 15kg. Alternatively, veterinarians can consider providing pet caretakers with a refilled epinephrine syringe for patients at risk fo reoccurrence. The disadvantage of this being the relatively short shelf life of only 3-4 months for a pre-filled syringe.

Prognosis
Initially, prognosis is always guarded as it is impossible to know if the reaction will be minor (localized) or develop into severe disease. Prognosis for patients with more sever reactions is fair to good providing prompt medical care is provided. Even those who develop significant complications have a chance of recovery.
Anaphylaxis will worsen with each episode and so the main goal after the pet has gotten over an initial episode is to prevent further episodes from happening. Once a diagnosis of anaphylaxis has been made and successfully treated, the key to management is to reduce the risk of re-exposure to the offending antigen.
With adequate preparation and close attention to clinical signs, treatment of anaphylaxis in dogs and cats can be a rewarding emergency scenario. So to have all this information on hand when you need it most, be sure to download the full anaphylaxis protocol at VetAPedia. For more useful ECC content, explore more of our emergency resources and patient care articles.




